ADF STAFF
The spark of inspiration came to Craig Parker during his long flight home to South Africa after visiting his grandmother in the United Kingdom for her 100th birthday.
“We weren’t sure whether she would survive this pandemic,” he told Discovery South Africa.
It was early in 2020, and England’s struggles with COVID-19 caused Parker to worry for South Africa.
“With all their resources and how much they were struggling,” he said, “[I realized] that we were going to be in real trouble.”
Parker, an anesthesiologist who left a 20-year career as a mechanical engineer in the mining industry to pursue his passion for medicine, decided to do something about the scarcity of ventilators and medical oxygen on the continent.
When he returned to his home in the Eastern Cape province, he wrote a post on Facebook asking for help from anyone who was interested in creating a new device.
Soon he had a team of volunteers: doctors, engineers, designers, 3D printing specialists and entrepreneurs.
They wanted to build a breathing aid, but unlike a ventilator, their goal was a noninvasive device that wouldn’t require intensive care unit beds, which were in short supply on the continent.
“I called in some of my mining buddies,” Parker told public health website Spotlight. “We had De Beers (a diamond manufacturing company) loan us two engineers at one point. We were tossing ideas around, building prototypes, testing them.
“I think it’s the hardest I’ve ever worked — like 18 hours a day.”
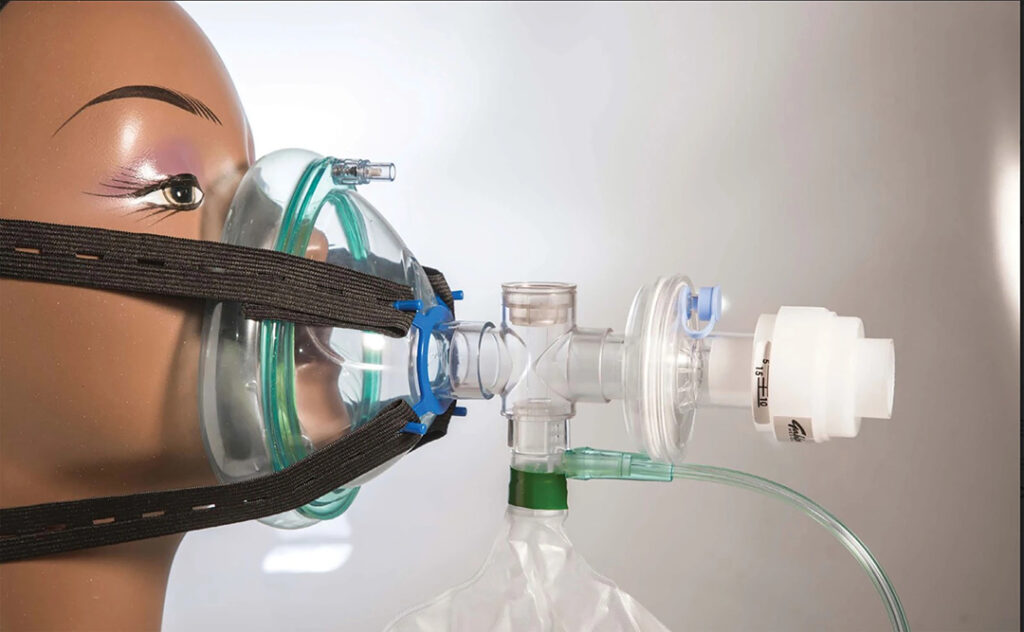
Seven weeks later, in March 2020, the Oxygen Efficient Respiratory Aid or OxERA was born. By December 2020, it was approved by South African health authorities for emergency use.
Using a well-sealed mask and an air pressure valve, a smaller amount of oxygen is needed to keep a patient’s lungs inflated.
Early in its development, the OxERA prototype was put to the test in Parker’s workplace, Frere Hospital in East London. During the first wave of the pandemic, the hospital admitted as many as 50 COVID-19 patients a day.
“I saw dramatic results,” Dr. Warren Gregorowski of Frere Hospital told Discovery. “I saw patients who were not coping on the standard oxygen masks actually get to high oxygen saturation levels.”
Parker and his colleagues had believed their device would work, but they were thrilled to see how well it performed.
“The device was still a prototype we were testing, but healthcare workers were desperate and finding them useful, and they were saving lives,” Parker told Spotlight. “So we were just making them and donating them to those who asked.”
Born in Zimbabwe, Parker was particularly pleased to see the OxERA used there.
“Zimbabwe, compared to South Africa, was so much worse,” he said. “Really, if you were anything beyond mildly ill there, it was a death sentence.
“They had no hope of big bulk oxygen supplies that could support high-flow nasal oxygen solutions. They didn’t have equipment or the skills to ventilate patients. So they used OxERA devices a lot.”
Parker, who did a year of community service in rural parts of the Eastern Cape after medical school, knew the OxERA would be a game-changer for remote health facilities.
“[OxERA] allows even the most basic facilities that are dependent on bottled oxygen or small oxygen concentrators to provide a higher level of clinical care than they are currently able to,” the product website says.
In September, Parker was honored as Rural Doctor of the Year by the Rural Doctors Association of South Africa.
“Dr. Parker’s leadership, knowledge and understanding of engineering, clinical and social fields was instrumental in the development of the OxERA product,” the association said in a statement.
His device also was listed in the World Health Organization’s 2022 Compendium in the category for “innovative health technologies for low resource settings.”
While the OxERA has been credited with saving hundreds of lives, Parker demurred and deflected attention to the “incredible volunteers … complete strangers” who came together to breathe life into his idea.
“Perhaps I am an average engineer and an average doctor,” he told Spotlight. “But this combination of skills is quite unique, and they were hugely beneficial during COVID.”